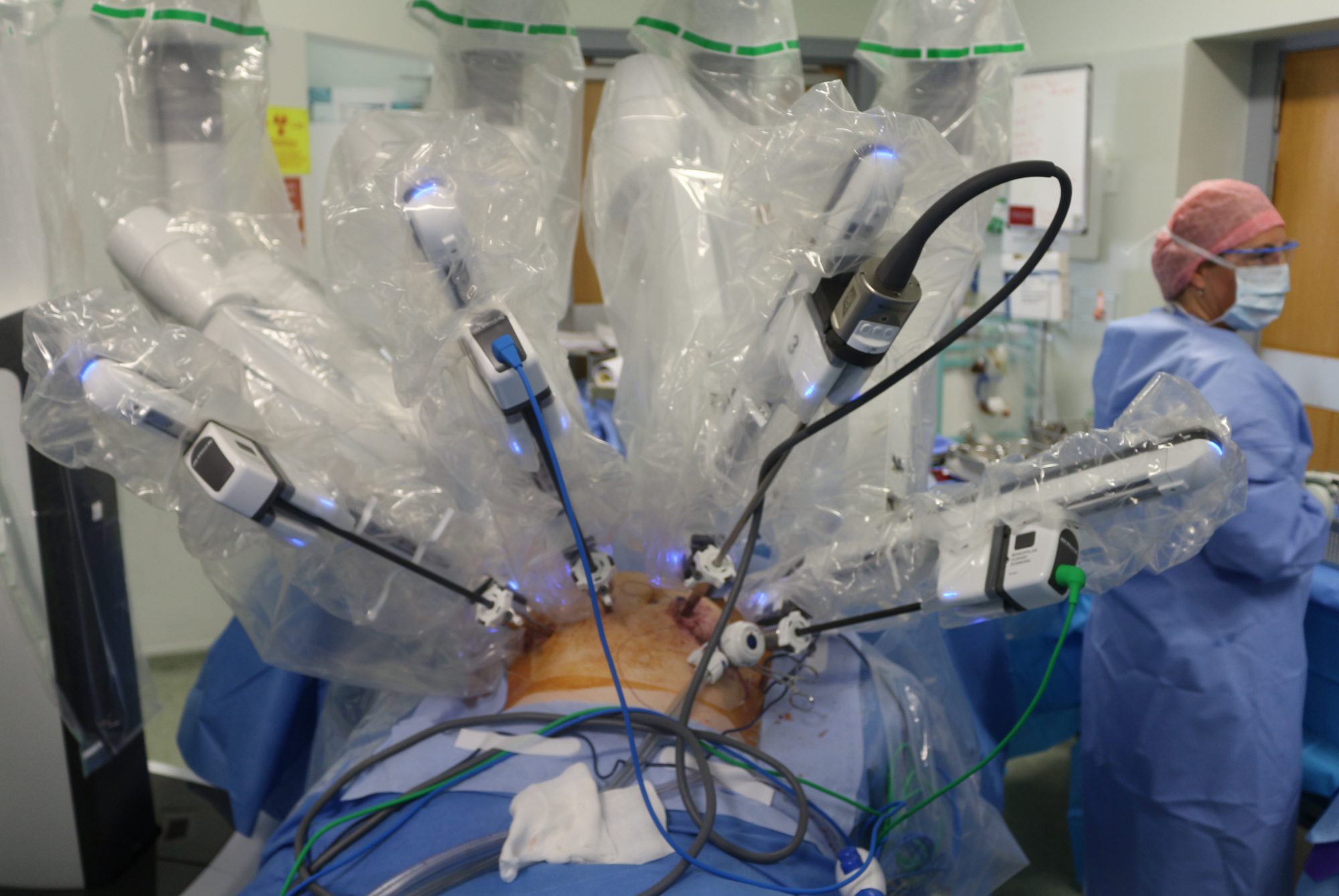
100 Robotic Surgery Cases Complete at University Hospital Limerick
1 Year of the robotic Assisted Surgery Program
ULGEMS students visit the DaVinci Robot
Great to have some of the 3rd and 4th medical students from University of Limerick Graduate Entry Medical School visit us at Theatre 7, University Hospital Limerick. Their enthusiasm for the robotic surgery project is evident from the video below.
Overview of robotic surgery at ULH
Limerick cancer survivor: ‘I owe an awful lot to JP the UHL robot’
 by Fintan Walsh 16 Sept 2017
by Fintan Walsh 16 Sept 2017
Raymond McNamara had a speedy recovery, and was back to work within a number of weeks
WHEN RAYMOND McNamara’s consultant told him a day before his cancer surgery that a robot was going to remove his kidney, he immediately thought it was a joke.
But that all changed when the 60-year-old Janesboro man was wheeled into the theatre and introduced to the four-armed Da Vinci robot last October.
The Da Vinci Xi dual console surgical robot — the only one of its kind in the Irish public health system — is the latest medical technological innovation that can operate on the most complex of cancer sites.
So far, the robot has operated on approximately 90 patients from all over the country since it was first docked in June 2016. And Raymond was one of the first patients to go under its knife for kidney cancer.
On the morning of September 10, Raymond was crossing the road on O’Connell Street to his workplace Don O’Malley and Partners, when the first symptoms of his life-changing illness “came out of the blue”.
“I found myself dying to go to the toilet. And when I went into the building, went straight up to the toilet, there was blood.”
“It wasn’t painful. It just felt very hot. And for the whole day, anyway, I was going up and down to the toilet, and it just started flowing. I went to the doctor the following morning, and he said: ‘You could have a kidney infection’ or something like that.”
Presuming that it was an infection, Raymond started his course of antibiotics, and was told to report back to the GP if the symptoms hadn’t cleared up by that Friday.
But the symptoms and the agony grew worse, day by day, and climaxed that Thursday, he says.
“I had to go to the Regional that Thursday, the pain was so intense. I couldn’t go to the toilet as blood clots were after forming. I found out much later on that the kidney was leaking blood because the tumour was after growing so big that it was ready to pop. And if it did pop, I would have been goosed,” a calm Raymond explains.
After spending a number of days at UHL, the patient thought that he was on the mend and ready to be discharged, until the registrar broke the bad news.
“The registrar came into me and said: ‘Look, we got the results of the scan’ and he said: ‘Basically, you have cancer in the kidney.’
“I asked him: ‘So what do I do from here?’ I was really straightforward about it. And he told me that they could remove the kidney completely, and that I could live with one.”
He admits that the first thing that went through his mind was his brother, who passed away at the age of 59.
He said to himself: “‘Oh Jesus, I am going to follow soon.’ You know the way you might think that? You would be thinking for the worst. But then when you settle down, you realise it might not be too bad.”
He adds that his his wife Mary, his two daughters and son also thought the worst at the beginning, but the registrar was able to put them at ease and explain his treatment.
Even then, he did not know that he was going to be on the operating table, with a man-controlled robot shadowing over him.
“It was about a day or two before it, I was told about it. I was told in a joking fashion, like: ‘Ah, we’ll see what the robot will do’ and I was like: ‘Hah?’ I didn’t think they had one.”
“And when I went up to the surgery, I didn’t know what to expect, I didn’t know what kind of a robot I was going to see. I was in the pre-assessment in the waiting area, and everything would be going through your mind. The surgeon then came in, he was making jokes and putting me at ease, and I laughed along with him.”
And then Raymond was wheeled into the operating room, where he met the Da Vinci surgical robot, who has been nicknamed “JP”, after billionaire philanthropist JP McManus.
The robot, which cost €2.6m, was donated by the JP McManus Benevolent Fund in early 2016.
Once the facility is docked, it is then operated by a maximum of two fully-trained surgeons in a separate console or room, who can make minimally invasive 8mm incisions via the robot.
After a successful nephrectomy — the complete removal of a kidney — Raymond had a speedy recovery, and was back to work within a number of weeks in November.
If this had been carried out without the aid of a robot, the period of convalescence could have been two to three times’ longer, he reckons.
The proud grandfather-of-four says that there could have been a different outcome if he had not received the initial symptoms on that morning in September.
“If I hadn’t got that warning, the morning I went to work, I wouldn’t be here to explain it to you. I didn’t know about it, it was growing on me for months, probably. And there was no explanation as to why it happened. I asked the surgeon if it was anything that I was doing, and he said: ‘No, it just happens.’”
He says that he is equally grateful for the “brilliant timing” of JP the Robot’s arrival at the Dooradoyle hospital.
“I was extremely grateful. I owe an awful lot to ‘JP’, as I like to call him. It is a tremendous facility.
“The people who get to use that machine are extremely lucky, and if they were sitting here today, I am sure they would be saying the same thing. I am just delighted that it was there, it was just brilliant timing,” he says with a smile.
And after being given a new lease of life, Raymond was able to celebrate his 60th birthday with his family just last month.
“My attitude towards life changed a bit and my outlook changed too. Life is life, you make the most of it, and I am grateful that I am still here.”
Link to Original Article http://bit.ly/2xh9Kho
Leading Physician to Deliver Sir Peter Freyer Memorial Lecture at NUI Galway
Monday, 21 August 2017 by Marketing and Communications Office, NUI Galway

Pictured are Michael F. Collins, MD and Chancellor of the University of Massachusetts Medical School & Senior Vice President for Health Sciences at the University of Massachusetts with Calvin Coffey the Foundation Chair of Surgery in University of Limerick and University Hospitals Limerick Group.
NUI Galway will host the 42nd Sir Peter Freyer Memorial Lecture and Surgical Symposium, the largest Surgical Conference in Ireland, from 1-2 September.
The annual event provides a platform for healthcare professionals to present their research and clinical work, and allows for the merging of both scientific and clinical information. It is named in memory of the Galway-born surgeon, Sir Peter Freyer, who performed the first successful surgical operation to remove an enlarged prostate in 1900. It comprises multiple research and education sessions across the various surgical subspecialties, two keynote addresses and discussion around the future of Irish Surgery.
 Michael F. Collins, MD is Chancellor of the University of Massachusetts Medical School & Senior Vice President for Health Sciences at the University of Massachusetts will deliver the Memorial Lecture entitled ‘In Search of the Tossed Cap: Following Medicine’s Privilege’ on Friday, 1 September. Dr Collins currently oversees the University of Massachusetts system-wide health and life sciences portfolio, charged with leading strategic initiatives to strengthen the university’s efforts in the area and to engage more fully with the Commonwealth’s dynamic health and life sciences sector. Dr Collins is actively engaged in service to the Commonwealth of Massachusetts and has amassed vast experience in governance of not for profit and educational entities. Currently, he serves on the boards of UMass Memorial Health Care, Massachusetts Biomedical Initiatives, The American University of Beirut, Commerce Bancshares Corp., Worcester Regional Chamber of Commerce, Greater Worcester Community Foundation and the Higher Education Consortium of Central Massachusetts. He is a Board Certified Physician in Internal Medicine and a Fellow of the American College of Physicians.
Michael F. Collins, MD is Chancellor of the University of Massachusetts Medical School & Senior Vice President for Health Sciences at the University of Massachusetts will deliver the Memorial Lecture entitled ‘In Search of the Tossed Cap: Following Medicine’s Privilege’ on Friday, 1 September. Dr Collins currently oversees the University of Massachusetts system-wide health and life sciences portfolio, charged with leading strategic initiatives to strengthen the university’s efforts in the area and to engage more fully with the Commonwealth’s dynamic health and life sciences sector. Dr Collins is actively engaged in service to the Commonwealth of Massachusetts and has amassed vast experience in governance of not for profit and educational entities. Currently, he serves on the boards of UMass Memorial Health Care, Massachusetts Biomedical Initiatives, The American University of Beirut, Commerce Bancshares Corp., Worcester Regional Chamber of Commerce, Greater Worcester Community Foundation and the Higher Education Consortium of Central Massachusetts. He is a Board Certified Physician in Internal Medicine and a Fellow of the American College of Physicians.
Professor Calvin Coffey is the Foundation Chair of Surgery in University of Limerick and University Hospitals Limerick Group. Professor Coffey will deliver the State of the Art Lecture entitled ‘Da Vinci and Colorectal Surgery’ on Saturday, 2 September. Professor Coffey in 2016 pioneered robotic intestinal surgery in Ireland and led the team that set up the first multidisciplinary robotic program in Ireland. He is the chief author of the book Mesenteric Principles of Gastrointestinal Surgery: Basic and Applied Science. This book is the first reference test on the human mesentery, related diseases and surgical treatment strategies. He is editor in Chief of the journal, Mesentery and Peritoneum.
The Programme also features a Session on the Role of Research in Surgical Training discussing the optimisation of the potential and opportunities for all Surgeons and trainees to take part in research, acquiring necessary skills and methodology throughout their careers.
Professor of Surgery at NUI Galway, Michael Kerin, who is hosting the event along with his colleague Professor Oliver McAnena, said: “We are delighted to welcome Dr Collins and Professor Coffey to our University. Dr Collins is a sought-after motivational speaker, who draws from his decades-long experiences in academic medicine to frame the enduring role of physicians in a profession that continues to evolve from and be shaped by external forces.”
Professor Coffey has published ground-breaking research which has identified an emerging area of science having reclassified a part of the digestive system as an organ. Professor Coffey’s research proposes that the mesentery, which connects the intestine and the abdomen, is an organ. For hundreds of years it had been seen as a fragmented structure made up separate parts. Their lectures are the focal points of a large programme containing some of the best surgical research from this country”.
Limerick native Colin Peirce joins UL Hospitals Surgeon team
UL HOSPITALS Group has announced the appointment of Mr Colin Peirce, MD, FRCSI, as Consultant Colorectal/General Surgeon.

Mr Peirce graduated with first class honours in surgery from Trinity College Medical School, Dublin, in 2004 and previously worked in the UL Hospitals Group as a specialist registrar in general and colorectal surgery in 2012/13.
Mr Peirce said he was “very excited and honoured to join the robotic surgery team in Limerick in what is both a unique opportunity and program within the Irish health service”.
Commenting on the appointment this week, Colette Cowan, CEO, UL Hospitals Group said: “We are delighted to have been able to entice Mr Peirce home to join what we feel is one of the best, if not the best Department of Colorectal Surgery in the country.
Colin joins Mr David Waldron, Prof Calvin Coffey and Mr Eoghan Condon in what is a great combination of experience and dynamism -one that is proving of great benefit for our reputation as a teaching hospital, and more importantly for all the patients of the MidWest. We have great plans for robotic surgery here at UL Hospitals and Colin is a fantastic addition to the team. I wholeheartedly welcome him on behalf of all the staff here at UL Hospitals.”
TEDx The Mesentery
Published on 11 Jul 2017
Calvin has identified an emerging area of science having reclassified part of the digestive system as an organ. When asked what this discovery will mean for the future of medicine.
Calvin’s TEDx talk will explore the benefits of this new science and relevant implications. That will span across many sectors and professions.
Professor Calvin Coffey
holds a variety of medical positions, both academically and professionally. These are the following; Foundation Chair of Surgery, Professor of Surgery, Graduate Entry Medical School in the University of Limerick. Consultant Surgeon in Health Services Executive (HSE). Deputy Director, 4i Centre for Interventions in Inflammation, Infection and Immunity. Vice-Dean of postgraduate surgical education in RCSI for the mid-western region. Secretary of the Irish Association of Coloproctology. Council member of the Irish Hospital Counsultant’s Association and lastly, a James IV Travelling Fellow since 2011.
This talk was given at a TEDx event using the TED conference format but independently organized by a local community. Learn more at https://www.ted.com/tedx
http://thelancet.com/journals/langas/article/PIIS2468-1253(16)30026-7/fulltexthttp://dx.doi.org/10.1016/S2468-1253(16)30026-7
Eolas Magazine Robotic Surgery at UHL
Robotic surgery
eolas examines the robotic surgical services on offer to public patients and how surgery has been revolutionised by this technology.
The Robotic Assisted Surgery (RAS) Program at University Limerick Hospital is at the forefront of future surgery delivery. The hospital now offers the robotic surgery to all patients in the Mid-Western region. The control, accuracy and versatility provided by the console controlled instruments is unmatched. It is the most advanced form of keyhole surgery and is of the highest standard currently available globally.
During surgery, the Da Vinci robot is secured or ‘docked’ to the patient and has four working arms, each requiring only an 8mm skin incision, to which operating instruments are attached. Once docked, the surgeon who is positioned at a console nearby controls the robotic arms. The 3D view provided to the surgeon is unprecedented in surgery to date. The dual console allows two surgeons to operate simultaneously ensuring optimal decision-making and doubling the expertise.
Until the RAS Program was launched in May 2016, this type of surgery was only available in private health institutions in Ireland or patients had to travel abroad. The program was funded by the Mid-Western Hospitals Development Trust and the University of Limerick.
The Minimally Invasive Surgery (MIS) Forum has also been established to provide evidence of regulatory compliance. The team comprises of around 15 professionals with meetings focusing alternately on morbidity and mortality. The robotic team performed extensive research and training prior to introducing the program. This included surgeons who travelled to the United States and Australia to complete robotic training fellowships.
Surgical approaches and techniques have changed dramatically over the last 25 years. Traditionally, patients with kidney or colorectal cancer would have needed a large open incision (20cm or more) to remove the affected organ. However, keyhole surgery revolutionised surgical practice. Robotic surgery has further enhanced keyhole surgery benefits by allowing a level of technical precision that is not possible in traditional surgery.
Benefits for the health system
Major surgery for kidney or colorectal cancer with use of robotics has a shortened recovery time of around four days. Patients lose a minimal amount of blood during surgery, need less pain medication post operation, are mobilising on the first postoperative day and have a reduced length of stay in hospital.
This enhances patient flow through the hospital therefore benefiting all patients, who have had either robotic or traditional surgery, in the hospital due to the freeing up of occupied bed days. On average, three robotic operations take place each week in the hospital. Through the reduction in length of hospital stays and other savings such as instrumentation, the program runs at cost neutral.
The dual console is the only one of its kind in Ireland and allows for training of future surgeons. The surgeons are positioned side-by-side and the control of the surgical instruments can be swapped between both surgeons. UHL can also broadcast live surgery within the hospital to its junior doctors. This provides an educational program for medical staff, nursing staff and students.
The program so far has focused on the colorectal and urological fields. Gynaecological, endocrine and pelvic floor surgeons are undertaking robotic training and these specialities will lead to further utilisation of the robot and further opportunities for patients to benefit from the cutting edge of surgical technology.
Link to original article http://www.eolasmagazine.ie/robotic-surgery/
Anatomy for Robotic Colorectal Surgery
Recent research with a focus on anatomy for robotic colorectal surgery
The mesentery: structure, function, and role in disease
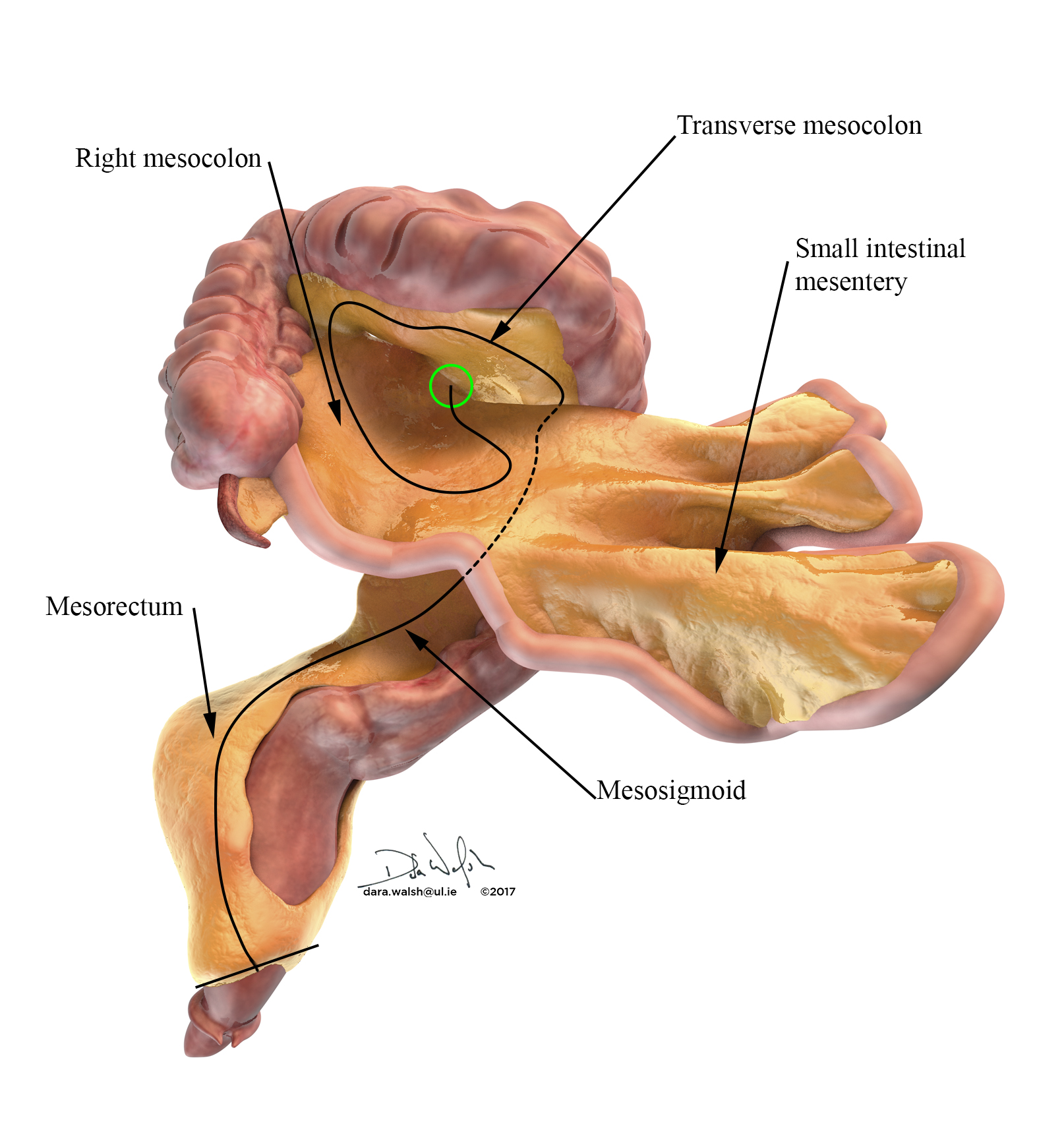
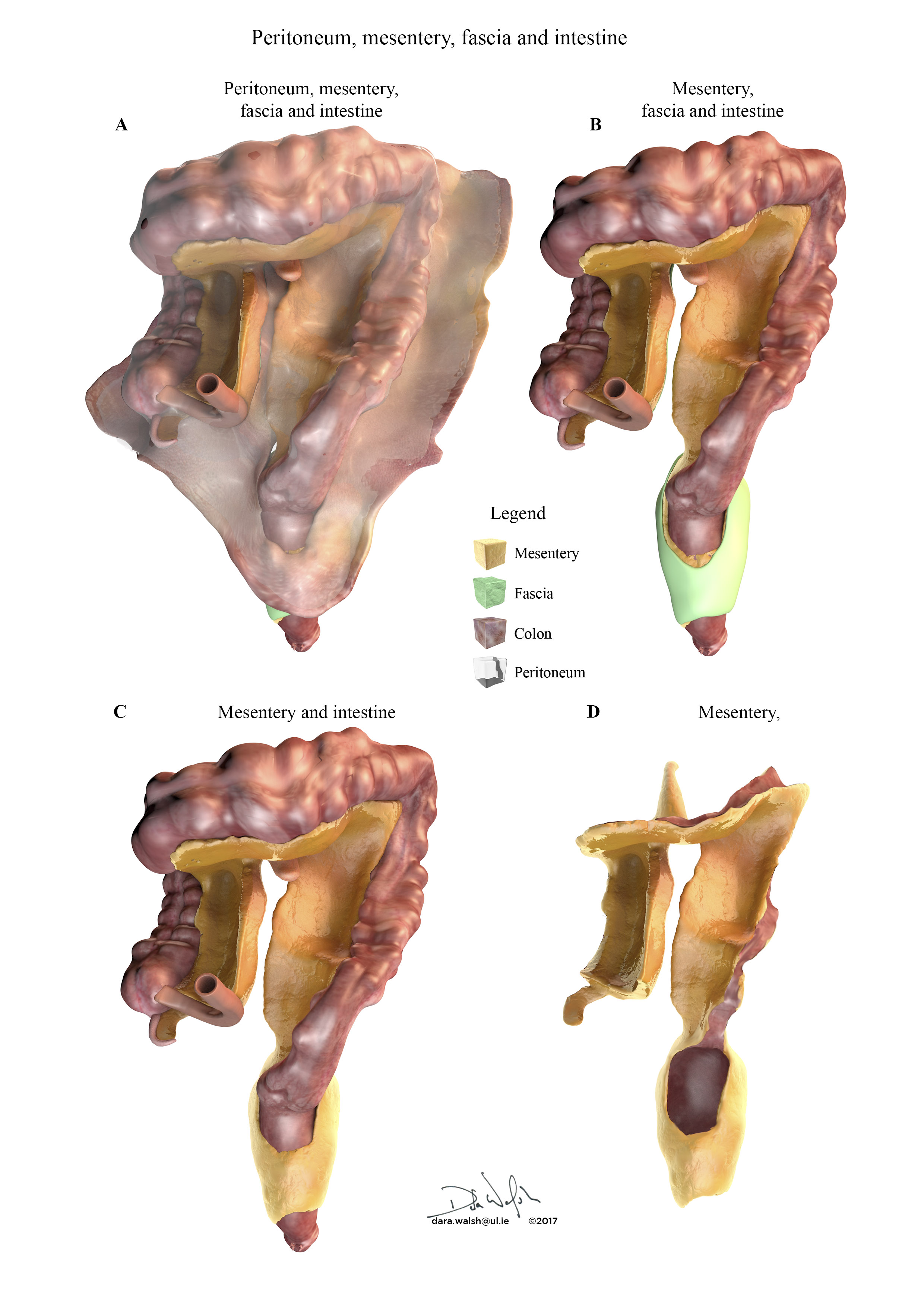
http://thelancet.com/journals/langas/article/PIIS2468-1253(16)30026-7/fulltext
http://dx.doi.org/10.1016/S2468-1253(16)30026-7
Learn more ar www.mpgs.ie